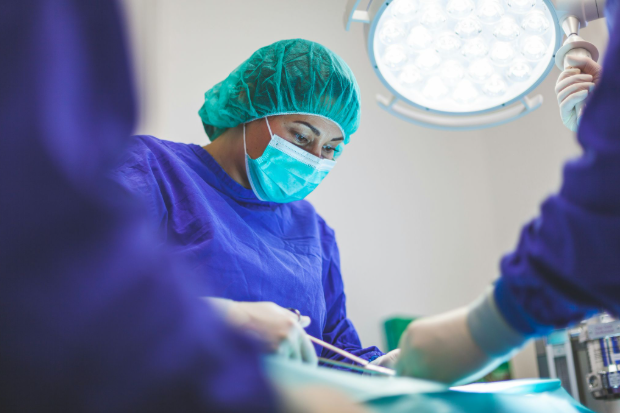
How to Recognize Strain Before It Becomes Pain or Performance Loss
Clinicians often work through discomfort without realizing how much physical strain is building beneath the surface. In surgical suites, dental practices, procedural centers, and outpatient environments, musculoskeletal fatigue frequently develops gradually rather than appearing as sudden pain.
Because healthcare professionals are trained to focus on patient care and task precision, subtle physical warning signs are commonly ignored or normalized. Many clinicians do not identify fatigue until the end of the day, after multiple procedures, or when symptoms begin to interfere with comfort and performance.
The challenge is that by the time pain becomes obvious, fatigue has often been accumulating for weeks, months, or longer. Recognizing earlier signals can help reduce long-term strain and support more sustainable clinical performance.
According to the National Institute for Occupational Safety and Health (NIOSH), musculoskeletal disorders are strongly associated with repetitive movement, forceful exertion, and sustained awkward posture, all of which are common in healthcare environments.
Learn how structured cervical support can help reduce early fatigue signals and improve endurance across long clinical schedules.
Why Clinicians Miss Early Fatigue Signals
Musculoskeletal fatigue often develops silently. It does not always begin with sharp pain or obvious limitations. Instead, it usually starts as subtle changes in posture, endurance, movement quality, or concentration.
Healthcare professionals frequently overlook these signals because:
- Attention is directed toward patient outcomes.
- Short-term discomfort is considered normal for the job.
- Symptoms fade temporarily after rest.
- Fatigue builds gradually over time.
- Work culture often rewards pushing through discomfort.
This means early-stage strain can continue unnoticed until it becomes harder to reverse.
Sign 1: Frequent Neck Repositioning During Procedures
One of the earliest indicators of cervical fatigue is repeated repositioning of the head and neck.
A clinician may subtly:
- Lift the head and reset posture.
- Roll the shoulders
- Shift chin position
- Lean backward briefly between tasks.
These movements often occur unconsciously and indicate that the stabilizing muscles are tiring. If neck repositioning becomes more frequent later in the day or during longer procedures, cumulative cervical load may already be developing.
Sign 2: Shoulder Elevation Without Awareness
As neck muscles fatigue, the body often recruits nearby muscle groups to compensate. A common example is raised shoulders during concentrated tasks.
This may appear as:
- Tight shoulders during charting or procedures
- Elevated shoulder posture while using instruments
- Tension between the shoulder blades
- Reduced ability to relax the upper body
According to OSHA ergonomic guidance, compensatory posture patterns often develop when workstations or task demands exceed comfortable neutral positioning.
Shoulder elevation is often treated as stress when it may actually be an early fatigue signal.
Sign 3: Leaning Closer to the Work Area
When endurance drops, clinicians often move the head closer to the treatment field, monitor, or patient area.
This can happen because:
- Forward positioning feels easier than holding an upright posture.
- Visual focus increases under fatigue
- Core and cervical support decline over time
Although common, repeated forward head posture increases the mechanical load on the cervical spine and may accelerate fatigue. If a clinician consistently leans toward the end of shifts, it may indicate declining postural endurance.
Sign 4: Increased End-of-Day Stiffness
Pain is not always the first symptom of fatigue. Stiffness often appears earlier.
Common examples include:
- Neck tightness while driving home
- Shoulder stiffness after removing PPE
- Upper back tension at the end of clinic hours
- Feeling the need to stretch immediately after work
These signs suggest that muscles remained under sustained load throughout the day. If stiffness becomes a routine pattern, it may indicate that physical recovery is not keeping pace with workload demands.
Sign 5: Reduced Tolerance for Long Cases or Busy Schedules
Clinicians with early musculoskeletal fatigue may still perform at a high level, but their tolerance for demanding schedules often declines first.
Signs may include:
- Feeling drained earlier in the day
- Needing more recovery after procedures
- More noticeable fatigue during back-to-back cases
- Reduced energy during later appointments
This is an important warning sign because endurance loss often appears before significant pain.
Sign 6: Small Declines in Focus Under Load
Musculoskeletal fatigue is physical, but it can also affect mental efficiency.
As posture demands rise, clinicians may notice:
- Greater mental effort is required late in the day.
- Slower transitions between tasks
- Increased distraction from physical discomfort
- Reduced concentration during repetitive procedures
NIOSH has noted that physical fatigue and awkward postures can affect worker performance, especially in high-demand occupations that require sustained precision. These subtle cognitive effects often improve when physical strain is reduced.
Sign 7: Needing Constant Stretching to Get Through the Day
Stretching can be helpful, but needing to stretch repeatedly to maintain comfort may signal that the underlying workload exceeds current support.
If a clinician must constantly:
- Stretch the neck between patients.
- Roll the shoulders every hour.
- Stand up repeatedly to relieve discomfort.
- Use temporary fixes throughout the day.
Then fatigue may be accumulating faster than the body can recover. Stretching addresses symptoms, but it may not reduce the source of static load.
Why Early Action Matters
Waiting until pain becomes severe often means that strain has been present for an extended period. Earlier recognition allows clinicians and organizations to intervene before fatigue becomes chronic.
Benefits of early action include:
- Reduced long-term musculoskeletal stress
- Better daily comfort and endurance
- More consistent posture during procedures
- Lower risk of progression into persistent pain
- Improved sustainability across years of practice
Preventive ergonomics is typically more effective than reactive symptom management.
How Structured Support Helps Reduce Early Fatigue Signals
Many clinicians are told to improve posture, stretch more, or adjust their workstation. While useful, these strategies do not always reduce the muscular demand of sustained head and neck positioning.
Structured cervical support reduces the effort required to maintain posture during prolonged clinical tasks.
NekSpine is designed to assist the cervical spine during static work, helping reduce continuous muscular strain that can lead to fatigue signals such as stiffness, leaning, and repeated repositioning.
Potential benefits may include:
- Better endurance across long schedules
- Reduced neck and upper back fatigue
- More consistent posture during procedures
- Less end-of-day physical exhaustion
- Improved recovery after workdays
What Organizations Should Watch For
Hospitals, practices, and administrators should not wait for injury claims to recognize the risk of fatigue.
Early indicators across teams may include:
- Frequent complaints of stiffness rather than pain
- Staff needing more physical recovery time
- Increased discomfort during long cases
- High reliance on stretching or self-management
- Fatigue complaints late in shifts
These patterns may suggest a broader ergonomic issue rather than isolated personal discomfort.
Building a More Sustainable Clinical Career
Clinicians often accept physical fatigue as part of the profession, but chronic strain should not be considered inevitable.
Recognizing early warning signs allows individuals and organizations to act sooner, reduce preventable load, and support long-term performance.
The goal is not simply less pain. It is better endurance, stronger sustainability, and healthier careers.
Learn How Structured Support Reduces Early Fatigue Signals
If your team is noticing stiffness, declining endurance, or subtle posture breakdown during procedures, early intervention matters.
Learn how NekSpine can help reduce musculoskeletal fatigue signals, improve clinician endurance, and support healthier long-term performance in demanding clinical environments.