Surgeon Musculoskeletal Disorders: A Growing Threat to Workforce Sustainability
Work-related musculoskeletal disorders (MSDs) among surgeons have become a critical and measurable threat to modern surgical workforce capacity. Evidence across multiple specialties shows that prolonged static postures, sustained neck flexion, and constrained upper-back mechanics create cumulative biomechanical strain that directly affects surgeon longevity and performance. A landmark systematic review reports that approximately 49% of physicians experience back pain within a 12-month period, and 12% of them require practice modification, leave, or early retirement due to MSD symptoms. Specialty-specific studies reveal even higher prevalence: orthopedic and arthroplasty surgeons report MSD rates consistently above 80–90%, highlighting the severity of ergonomic stress in high-demand operative environments.
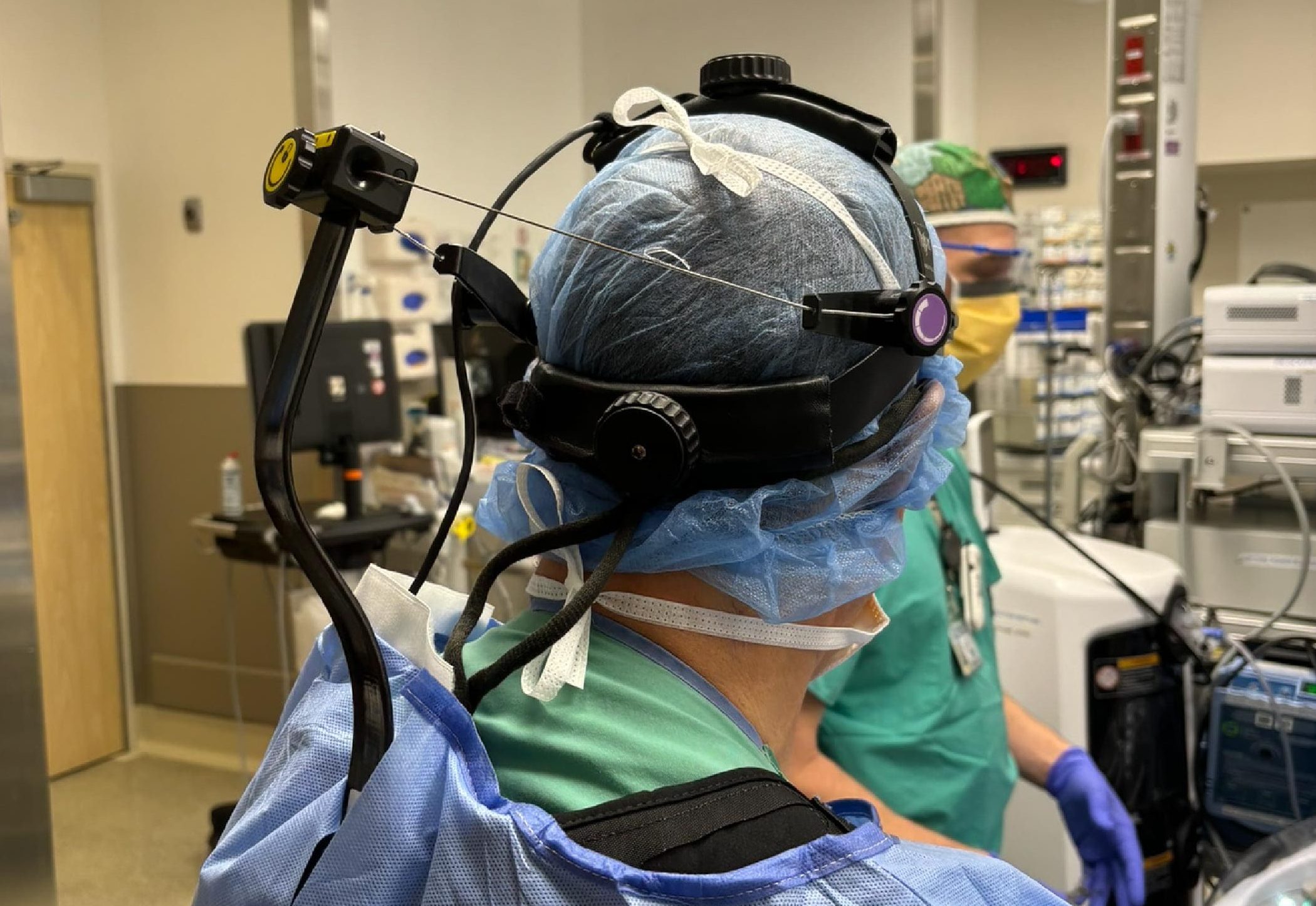
This growing burden has accelerated interest in preventive, non-disruptive support technologies such as the NekSpine® ergonomic support system, designed to reduce cervical loading during posture-intensive procedures.
These epidemiological findings demonstrate that MSDs are not isolated clinician-health events—they represent an escalating operational risk for hospitals dependent on high-margin surgical service lines.
How Fatigue and Pain Influence Performance and Patient Outcomes
Surgeon discomfort is not merely a wellness issue; it is closely linked to technical performance, cognitive bandwidth, and overall intraoperative precision. Studies analyzing surgeon fatigue show that physicians may be significantly fatigued for nearly half of their waking hours, and that longer OR days correlate with slower reaction time, decreased situational awareness, and higher risk of micro-errors. Ergonomic strain and cervical loading have also been associated with compromised posture stability, reduced fine-motor control, and diminished operative endurance.
Over time, persistent musculoskeletal pain can shorten clinical careers by accelerating burnout, reducing weekly case volume, and forcing early departure from physically demanding specialties. For high-complexity cases—cardiothoracic, neurosurgery, complex orthopedics—any decrement in surgeon endurance directly affects patient throughput and service-line efficiency.
If your institution is exploring ways to reduce fatigue and protect long-term surgical performance, contact us to learn how posture-support solutions can be integrated into existing OR workflows.
The Financial Weight of Work-Related MSDs for Health Systems
The economic implications of surgeon MSDs extend well beyond direct medical claims. In the United States, MSDs contribute an estimated $13–54 billion annually in combined direct and indirect costs. Neck and central nervous system–related workers’ compensation claims alone commonly average $70,000–$90,000 per incident, excluding downstream consequences such as:
- Cancelled or delayed OR days
- Reduced case volume and throughput
- Productivity loss
- Recruitment and onboarding costs for replacement surgeons (often exceeding $250,000 per specialist)
In hospitals where surgical procedures drive a disproportionate share of contribution margin—e.g., programs with US$8,000–$22,000 per case—even a small reduction in surgeon availability translates into substantial financial impact. A single cancelled OR day in cardiothoracic or neurosurgery can exceed the total cost of multi-year preventive ergonomic interventions.
This economic reality reinforces the need for proactive occupational-health strategies that prevent MSDs rather than respond to them after injury occurs.
Passive Exoskeleton Support as an Engineering Control for MSD Risk
Organizations increasingly recognize that administrative fixes—break scheduling, ergonomic training, or posture reminders—are insufficient for controlling real-world cervical and thoracic loading during long operative days. A more impactful approach is the introduction of engineering controls that physically reduce mechanical strain.
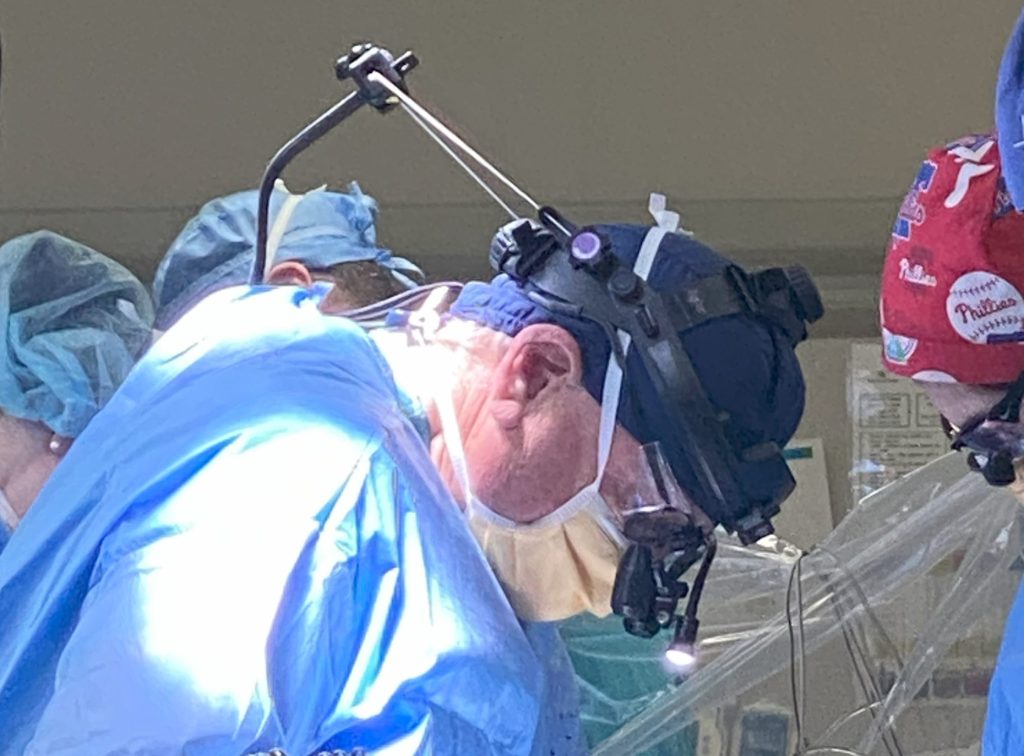
Passive upper-body support exoskeletons, such as the carbon-fiber framework evaluated in recent multicenter studies, offer 30–60% offloading of effective head weight, reducing cervical loading during posture-intensive procedures while preserving full range of motion and visualization. Independent evaluations, including a 2025 ergonomics assessment and a pilot published in Annals of Surgery, found:
- Reduced neck and back muscle activity (EMG)
- Decreased perceived exertion
- Improved posture endurance
- No negative impact on dexterity or workflow
These findings are consistent with the broader literature showing that passive support systems can significantly reduce neck/trapezial fatigue during simulated surgical tasks.
If you’re interested in evaluating passive support systems within your specialty—ENT, plastics, cardiothoracic, or neurosurgery—reach out to schedule a structured pilot.

Why Preventive Ergonomic Interventions Generate High Return on Investment
From a Health Economics and Outcomes Research (HEOR) perspective, passive exoskeleton support represents a capital-efficient method of reducing mechanical risk exposure in the surgical workforce. Internal modeling shows:
- A 3–9 month payback period
- 250–400% ROI within two years when deployed across a service line
- Claim avoidance value where preventing a single $25,000–$30,000 neck/spine injury can offset ~10 device acquisitions
- Even 0.5% fewer lost OR days can produce meaningful financial return
Most importantly, preventive support protects surgeons before injuries accumulate—preserving workforce longevity, maintaining case capacity, and preventing workflow disruptions. These outcomes align with institutional priorities across ESG metrics, safety-culture development, and clinician-wellness initiatives.
If your hospital is integrating ergonomic risk reduction into its ESG or workforce-sustainability strategy, we can provide specialized HEOR modeling tailored to your service-line data.
Addressing an Occupational Risk That Can No Longer Be Ignored
Surgeon MSDs represent a measurable clinical, operational, and financial threat to health systems. High rates of neck and spine pain, growing evidence linking fatigue to performance variability, and escalating injury-related costs all point to the same conclusion: preventive ergonomic solutions are now essential.
Passive neck and upper-back support technologies offer a non-disruptive, clinically validated approach to reducing cervical load and improving operative endurance without interfering with surgical technique. For institutions seeking to maintain surgical throughput, support clinician longevity, and strengthen occupational-health infrastructure, these systems provide both an evidence-based and economically sound path forward.